It can be easy to forget that the human skin is an organ. It’s also the largest one and it’s exposed, charged with keeping our inner biology safe from the perils of the outside world.
But Michigan State University’s Sangbum Park is someone who never takes skin or its biological functions for granted. He’s studying skin at the cellular level to better understand it and help us support it when it’s fighting injury, infection or disease.
In the latest installment of that effort, Park, who works in IQ — MSU’s Institute for Quantitative Health Science & Engineering — has helped reveal how the skin’s immune cells organize themselves to ward off would-be intruders. Park and his colleagues published their work on May 6 in the journal Nature Cell Biology.
“Immune cells are the soldiers of our body. In our skin, that army is maintained according to two factors: density and distribution,” said Park, an assistant professor in the Department of Medicine and Department of Pharmacology and Toxicology.
“We need enough immune cells to cover the whole area of our skin uniformly for proper protection. Otherwise, our skin would be vulnerable to damage and infection,” Park said. “As sensible as that might sound, it was unclear how, or even if, these immune cells were organized before this study. Many researchers thought the cells’ distribution was random.”
Skin’s immune cells have a history of being misunderstood. Many people don’t realize that our outermost layer of skin, the epidermis, is home to immune cells. And when the German scientist Paul Langerhans first discovered one type of these immune cells in the late 1800s — cells that are now called Langerhans cells — he mistook them for cells from our nervous system (to be fair, they do have a similar morphology).
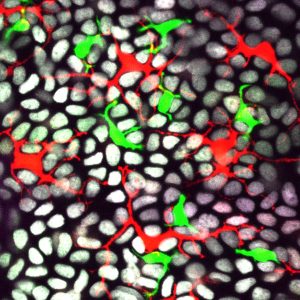
This microscope image shows how the skin’s immune cells, shown in red (Langerhans cells) and green (dendritic epidermal T cells) arrange themselves among gray epithelial cells in live mice. Credit: Sangbum Park
To bring more clarity to how skin’s immune cells do their jobs, Park and his co-workers used state-of-the-art microscopy tools. The researchers illuminated how live immune cells arranged themselves in the skin of mice, a popular animal model with a skin biology similar to that of humans.
“IQ has so many advantages for a young investigator like me,” said Park, who joined MSU in January 2020. Just two months later, he had to start working from home due to the coronavirus pandemic. But thanks to IQ’s strong microscopy core, Park’s team was able to work almost immediately as restrictions lifted.
“I didn’t have to wait to set up microscopes in my own lab or train my students how to use them,” he said. “At IQ, we already have many different microscopes for a wide range of animal models.”
As a result, Park’s team is revealing the skin’s structure and function like never before. Having validated these new techniques and observing how immune cells are organized in the healthy skin of mice, Park’s team can start probing new questions about how skin heals.
“My lab is interested in how skin regenerates and recovers from injury,” he said. That injury could be a cut, an infection, an allergic reaction or an even more persistent disorder, such as psoriasis. “We can answer so many questions with our intravital imaging technique that you just can’t with conventional methods.”
Note for media: Please include a link to the original research in your online coverage: https://www.nature.com/articles/s41556-021-00670-5
- Via MSUToday



